First bite syndrome chemotherapy7/9/2023 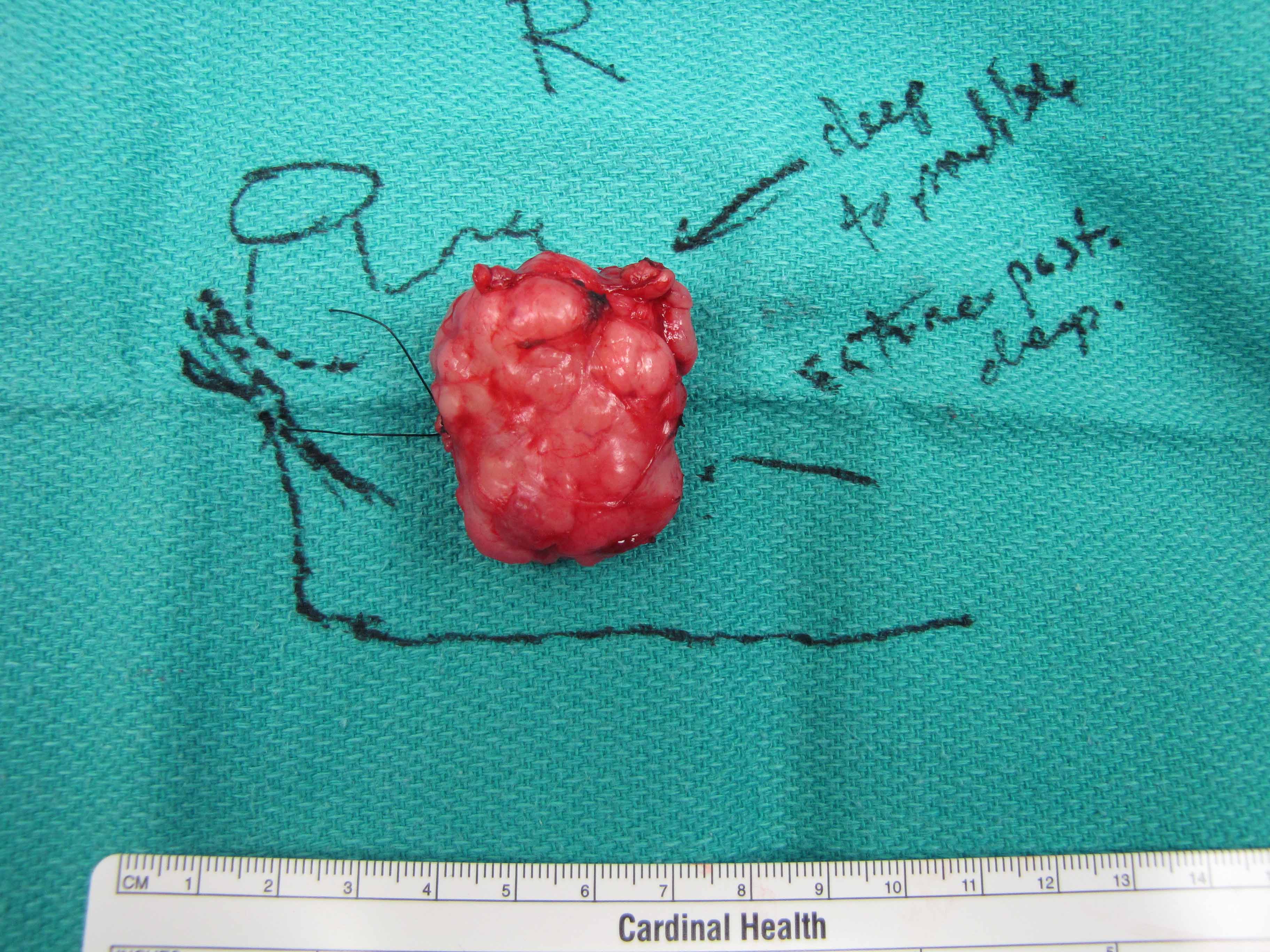
And the comparison of these three T-cell based immunotherapies is summarized in Table 1. Bispecific T-cell engager (BiTE) stands out as a novel subclass of T-cell engaging bsAbs with promising clinical results in the treatment of cancers. The other alternative approach to redirect T cells against target cells is T-cell engaging bsAbs with unique function engaging TAAs on cancer cells and cell surface molecules on T cells. The preparation of CAR T Cells primarily includes isolation of T cells from patients, genetic modification of T cells, expansion of T cells in vitro, and infusion of edited T cells to patients, however, which is a complex and time-consuming process. CAR T-cell therapy is a newly developed adoptive cell therapy by genetically engineering T cells to express a CAR comprising intracellular T-cell signaling domains and an extracellular antigen-recognition structure targeting tumor-associated antigens (TAAs), redirecting and activating T cells to eradicate malignant cells specifically. 
A major reason for this is the lack of a sufficient number of tumor-infiltrating immune cells (TILs), primarily T cells, in the tumor site, which is referred to as exhibiting cold phenotype. They hamper the tumor immune escape by blocking key immunosuppressive molecules such as programmed cell death 1 (PD-1) and its ligand (PD-L1) and releasing the “brake” of cytotoxic T cells to eliminate tumor cells, however, response rates of ICIs remain limited. ICIs have revolutionized cancer treatment in the clinic, especially in several advanced solid tumors, for instance, melanoma and non-small-cell lung cancer. Depending on the mechanisms of action, T cell-based cancer immunotherapies can be mainly divided into two classes: one against immunosuppressive factors represented by immune checkpoint inhibitors (ICIs), the other one focusing on immunostimulatory pathways represented by chimeric antigen receptor (CAR) T cells and T-cell engaging bispecific antibodies (bsAbs). T cell-based cancer immunotherapies have transformed the clinical practice of cancer treatment by targeting and mobilizing T cells to eradicate malignant cells. In this review, we depict the landscape of BiTE therapy, including clinical advances with potential response predictors, challenges of treatment toxicity and resistance, and developments of novel immune cell-based engager therapy. In particular, immunotherapies focusing on innate immunity have attracted increasing interest and have shown promising anti-tumor activity by engaging innate cells or innate-like cells, which can be used alone or complement current therapies. Thus, modification of antibody constructs and searching for combination strategies designed to further enhance treatment efficacy as well as reduce toxicity has become an urgent issue, especially for solid tumors in which response to BiTE therapy is always poor. However, major mechanisms of resistance to BiTE therapy are associated with antigen loss and immunosuppressive factors such as the upregulation of immune checkpoints. BiTE therapy represented by blinatumomab has achieved impressive efficacy in the treatment of B cell malignancies. 
BiTE is a bispecific antibody construct with a unique function, simultaneously binding an antigen on tumor cells and a surface molecule on T cells to induce tumor lysis. To address this limitation, strategies for redirecting T cells to treat cancer are being intensively investigated, while the bispecific T cell engager (BiTE) therapy constitutes one of the most promising therapeutic approaches. T cell-based immunotherapies have revolutionized treatment paradigms in various cancers, however, limited response rates secondary to lack of significant T-cell infiltration in the tumor site remain a major problem.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
